INFECTIOUS INFLAMMATORY DISORDERS
REACTIVE LYMPHADENOPATHY
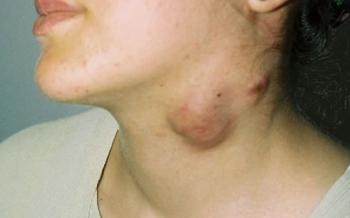
Enlargement of lymph nodes in response to antigen or infiltration. It can be acute or chronic, localized or widespread. They are normal-sized or slightly enlarged, well-circumscribed, multiple oval-shaped nodes.
In etiology; viral, bacterial, parasitic or fungal infections, chemical drugs or foreign antigens may be causative agents. Fever, rapid growth, pain, tenderness, erythema suggest inflammatory etiology. Reactive viral lymphadenopathy is the most common cause of adenopathy in children. These masses are usually associated with upper respiratory tract infection (URTI) symptoms. The most common viral agent; adenovirus, rhinovirus and entrovirus. These reactive lymphadenopathies (LAP) regress in 1-2 weeks. Treatment is usually observation. Adenopathies larger than 1 cm that do not regress in 4-6 weeks are considered pathological. If the adenopathy is persistent, a biopsy may be taken considering other causes such as fungal, granulomatous, or neoplastic.
In computed tomography (CT); homogeneous, well circumscribed, isodense or hypodense relative to muscle. In ultrasonography (USG), they are echogenic, oval-shaped nodes with vascular hilus. Contrast-enhanced computed tomography (CT), which is the most appropriate imaging, distinguishes reactive lymphadenopathy from suppurative and separates abscess from cellulitis. Cystic or suppurative intranodal changes are detected by contrast. Neck Doppler and USG were performed in 185 of 210 pediatric patients with acute inflammatory neck mass, CT was performed in 25 patients, and USG provided sufficient information in 184 of 185 patients (99.5%). The superiority of CT over USG; It shows both superficial and deep neck, it is more determinant in the spread of infection on anatomical planes.
Ebstein-Barr (EBV) or infectious mononucleosis can cause rubbery, mobile, diffuse, lymphadenopathies larger than 2 cm. It is usually accompanied by enlargement of lymphatic tissues such as tonsils and adenoids. Patients with EBV have fever and pharyngitis. Adenopathy may persist for 4-6 weeks in inf.mononucleosis. Treatment is for support purposes.
The most common symptoms are firm, sometimes fluctuating, mobile, subcutaneous nodal masses. It is painful in bacterial adenitis and cat-scratch disease.
The causative microorganism; Staf.aeirus, group B.Streptococcus, Kavasaki disease in infants, Staf.aeirus, gr.A beta hem.streptococcus, atypical mycobacteria in the 1-5 age group, anaerobes, toxoplasma, cat scratch disease, tuberculosis in the 5-15 age group (Tbc) is in the foreground.
In the pathology of reactive lymphadenopathy; nonspecific reactive properties are seen. Microscopic examination reveals follicular hyperplasia, paracortical hyperplasia, sinus histiosis, and polymorphic features of lymphoid cells at different stages.
In treatment; If there is a bacterial cause, antibiotics are used. Spontaneous regression occurs if cat scratch is a factor.
FNAB or open biopsy is required if there are systemic symptoms with inadequate response to antibiotics, rapid growth, firm preauricular, supraclavicular, posterior cervical nodes, mediastinal-abdominal LAPs, fever and weight loss. In persistent adenopathies lasting 3-6 months, repeat FNAB is recommended to exclude lymphoma, metastasis or TB.
INFLAMMATORY DISORDERS WITH HIV
1. Cervical adenopathy: Cervical adenopathy is present in 12-45% of HIV patients, idiopathic follicular hyperplasia develops. As treatment, it should treat the underlying HIV infection.
2. Persistent generalized lymphadenopathy: It is adenopathy that occurs in HIV-infected patients without infection or neoplastic cause.
BACTERIAL LYMPHADENOPATHY
1. Suppurative lymphadenopathy
In suppurative lymphadenitis, there is pus formation within the lymph node. It is seen in any lymph node group as localization, mostly retropharyngeal, jugulodigastric, submandibular lymph nodes are involved. 1-4 cm with an abscess focus. They are morphologically ovoid or rounded, cystic-appearing, often with unclear margins.
In contrast-enhanced CT, which is the most appropriate imaging, there is an image of a hypodense, thick-sided lymph node, and obvious opacity (phlegmon, cellulitis) is seen in the adjacent fat and subcutaneous tissue. Abscess formation, irregular, low-density fluid image from the periphery. Central echogenicity is low in USG. Branchial cyst, nodal fat metaplasia, tbc. lymphadenitis, atypical mycobacterial lymphadenitis, necrotic metastatic nodes should be considered in the differential diagnosis.
Pharyngitis, sinusitis, salivary gland infections, dental and mandible infections play a role in the etiology. First, adjacent lymph nodes enlarge reactively, then turn into suppurative. If left untreated, the nodes will rupture, and if the immune system is weak, an abscess will develop.
It is most common in pediatric and young adults. In societies with low socioeconomic status, inflammatory diseases are the most common cause of neck mass. In a study conducted in Iraq, the rate was found to be 57.8% in the pediatric group. In a study conducted in India, the rate is 54%. In the USA, the inflammatory rate was found to be 27% in 464 pediatric neck masses. In a study covering all age groups in Turkey, the rate of inflammatory neck mass is 33.4%. Tbc. lymphadenitis was found to be the most common cause of inflammatory masses with a rate of 40.28%.
If a fluctuant neck mass is erythematous and hot, an abscess has developed, and drainage and aspiration are required.
clinical symptoms; painful mass in the neck, color and temperature change in the skin, fever, poor oral intake. In the blood count, leukocytes and sedimentation were increased. The causative bacteria are the same as the reactive adenopathy micro-organisms.
As microscopic features in pathology; acute inflammatory cell infiltration, background necrosis, presence of neutrophils are observed.
Prognosis; conglomerated suppurative nodes result in abscess formation and rupture.
In the treatment, antibiotics for the primary source, incision in large suppurative nodes or abscesses, drainage, excision in atypical mycobacterial adenitis are recommended.
Toxoplasmosis
Toxoplasmosis is a cause of cervical adenopathy that can be transmitted from cats to humans. Ingestion of oocyte extracts from undercooked meat or cat faeces causes toxoplasma gondii ingested through transplacental transmission, organ transplant, and blood transfusion. T.gondii is a protozoan parasite with worldwide distribution in all mammals. The most common infection with toxoplasma organisms in immunocompromised patients; It is a hard, non-tender, non-suppurative, cervical lymph node enlargement less than 3 cm found separately.
Encephalitis, pneumonia, and acute respiratory failure may develop in immunocompromised patients. Fever, malaise, myalgia, sore throat, rash, hepatosplenomegaly, and atypical lymphocytes in the circulation may occur. The prevalence of the disease varies according to the environment, climate, living animals, and level of sanitation. In the seroepidemiological scans performed in the USA between the ages of 6-49, T.gondii was found to be seropositive in 11%.
A biopsy is taken from the lymph node for diagnosis. The specific histological triad of fluoride-reactive follicular hyperplasia, epithelioid histiocyte clusters, and sinusoidal swelling with monocytoid B cells is diagnostic for toxoplasmic lymphadenitis. Diagnosis can be confirmed by serological tests or isolation of toxoplasma species obtained from biopsy material by polymerase chain reaction of deoxyribonucleic acid is also of increasing importance.
Treatment is unnecessary in immunocompromised individuals. Symptoms and lymphadenopathy spontaneously regress within weeks to a few months. Medical treatment with sulfonamides or pyrimethamine is used when treatment is required.
Tularemi
The causative agent is Francisella tularensis. It is transmitted by rabbits, ticks or contaminated water. Patients have tonsillitis and painful LAP with systemic symptoms such as fever, chills, headache, and fatigue. Tularemia can cause prolonged cervical lymphadenopathy in glandular, oculoglandular, ulceroglandular, or oropharyngeal form. In oropharyngeal tularemia, the tonsils may be lacerated and ulcers may develop in the oral mucosa. Large conglomerated unilateral or bilateral multiple egg-sized adenopathies are seen. Suppuration may develop in the lymph nodes.
There has been an increase in the number of bacterial tularemia cases in the last ten years in our country. Tuberculosis and tularemia lymphadenitis can be confused with each other clinically and histopathologically. The diagnosis of caseified granulomatous lymphadenitis is both Tbc. and Tularemia, the same histopathological findings are valid for both diseases. Caseified necrosis, absence of neutrophils, sometimes intracellular or extracellular granuloma, ARB findings are valid for Tbc. lymphadenitis. In tularemia, the margins of the granuloma are sharp, few giant cells are seen in it.
In a study conducted in Turkey, the presence of M. tuberculosis in patients with a pre-diagnosis of tularemia-related cervical lymphadenitis made an important contribution especially for a wide geographical region where both diseases are endemic. In this study, Tbc. Contrary to the situation stated in this study, lymphadenitis due to oropharyngeal tularemia due to the histopathological appearance after clinical and excisional biopsy, in some cases treated with penicillin and its derivatives due to acute tonsillopharyngitis and treated with penicillin and its derivatives, cervical TB. It is considered as lymphadenitis and patients can be misdiagnosed and followed up with long-term antituberculosis treatment. In a recent seroepidemiological study examining this issue in our country, when 1170 cases of cervical lymphadenitis thought to be the causative agent of M.tuberculosis were investigated, the presence of tularemia antibodies was shown in 79 (6.75%). In another study, the presence of Francisella tularensis and M.tuberculosis was investigated by PCR method in paraffin tissue block preparations of 32 patients diagnosed with histopathologically cervical TB lymphadenitis in Bursa and its surroundings. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. In a recent seroepidemiological study examining this issue in our country, when 1170 cases of cervical lymphadenitis thought to be the causative agent of M.tuberculosis were investigated, the presence of tularemia antibodies was shown in 79 (6.75%). In another study, the presence of Francisella tularensis and M.tuberculosis was investigated by PCR method in paraffin tissue block preparations of 32 patients diagnosed with histopathologically cervical TB lymphadenitis in Bursa and its surroundings. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. In a recent seroepidemiological study examining this issue in our country, when 1170 cases of cervical lymphadenitis thought to be the causative agent of M.tuberculosis were investigated, the presence of tularemia antibodies was shown in 79 (6.75%). In another study, the presence of Francisella tularensis and M.tuberculosis was investigated by PCR method in paraffin tissue block preparations of 32 patients diagnosed with histopathologically cervical TB lymphadenitis in Bursa and its surroundings. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. When 1170 cases with cervical lymphadenitis, which is thought to be the causative agent, were investigated, 79 (6.75%) of them showed the presence of tularemia antibodies. In another study, the presence of Francisella tularensis and M.tuberculosis was investigated by PCR method in paraffin tissue block preparations of 32 patients diagnosed with histopathologically cervical TB lymphadenitis in Bursa and its surroundings. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. When 1170 cases with cervical lymphadenitis, which is thought to be the causative agent, were investigated, 79 (6.75%) of them showed the presence of tularemia antibodies. In another study, the presence of Francisella tularensis and M.tuberculosis was investigated by PCR method in paraffin tissue block preparations of 32 patients diagnosed with histopathologically cervical TB lymphadenitis in Bursa and its surroundings. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. The presence of tuberculosis was investigated. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis. The presence of tuberculosis was investigated. Tbc. Tularemia was detected as positive by PCR method in cervical lymph node samples in 6 (19%) patients who received treatment with the diagnosis of lymphadenitis.
Tularemia is transmitted to humans by contaminated water and unchlorinated hot spring waters in Turkey and similar countries. The diagnosis is confirmed by serological tests and culture.
In the treatment of tularemia, streptomycin, gentamicin, ciprofloxacin, doxycillin or chloramphenicol for 10-21 days may be sufficient and effective.
Brucelloz
Brucellosis is a disease caused by brucellosis, a gram-negative bacillus. It is most common in children with unpasteurized milk. It is an endemic disease.
It is quite common among animals. It is more common in Konya, Diyarbakır and Şanlıurfa regions in our country. B.melitensis infection is common in rural areas and B.abortus infection is common in big cities.
Symptoms begin in the afternoon. The fever, which rises with chills and chills in the evening, decreases with profuse sweating towards the morning (Ondulan Ateş). Migrating joint-muscle pain and involvement may be observed. Multiple system involvement such as orchitis and meningitis can be seen. There is diffuse cervical lymphadenopathy, fever, malaise, and fatigue. The diagnosis is made by serology and culture. In the treatment, streptomycin, doxycillin, rifampicin, trimethoprim-sulfamethoxazole or tetracycline are used according to the clinical picture.
GRANULOMATOSIS DISEASES
Cat-scratch disease, actinomycosis, atypical mycobacteria, tuberculosis, atypical tuberculosis and sarcoidosis cause granulomatous adenopathy of the neck.
cat scratch disease
Bartonella henselae, the causative agent of cat scratch disease, is an organism that can cause granulomatous cervical lymphadenitis. This infection can be defined as conjunctivitis and preauricular lymphadenopathy (Parinauds' oculoglandular syndrome)(6). This disease is a relatively common infection in young children exposed to cats, especially kittens. Around the inoculation, there are isolated mobile, fluctuant, erythematous, warm, tender adenopathies larger than 2 cm, fever, and malaise. Lymphadenopathies are localized in the preauricular and submandibular regions.
Diagnosis is made by serological tests with indirect fluorescein antibodies. In the biopsy, small pleomorphic gram-negative rods are seen in samples that can be cultured under special conditions and in sufficient time, and bacilli are seen in Warthin-Starry staining. Cat-scratch disease is benign, usually well-limited. In immunocompromised patients, infection and adenopathy usually regress spontaneously within a few weeks to months, and antibiotic therapy is not indicated. Patients with acquired immunodeficiency syndromes such as AIDS may need lifelong suppressive therapy with a macrolide or tetracycline.
Actinomycosis
Oral cervicofacial actinomycosis is a rare infection characterized by soft tissue mass or multilocular abscess formation, destruction of normal tissue levels, and the presence of sulfur granules, either macroscopically or microscopically. Studies have shown that 50-90% of actinomycosis is localized in the head and neck region. Classically, it appears as a slow-growing, painless, firm, possibly submandibular mass. However, it can also be seen as a rapidly progressive, painful, fluctuant infection with fever and leukocytosis in the neck or face.
Infection is caused by an admixture of oral microorganisms dominated by Actinomyces israelii, a large, gram-positive anaerobic bacillus. Actinomycosis is more commonly seen in people with poor oral hygiene or mucosal trauma, and its incidence has decreased with the age of antibiotics. Abscess formation enlarges with local invasion. It can pass to the brain and lungs by hematogenous route, lymphoid spread is rare.
In a case report made in our country, a 2 cm tumor in the submandibular region adjacent to the painless submandibular gland that did not respond to antibiotic treatment. sized lymphadenopathy was excised, and microabscesses with thick fibrous capsule, fibrous bands in the center between lymphoid follicles and characterized by actinomyces sulfur granules were detected in the pathology.
Abscess drainage is not needed in treatment. Prolonged antibiotic therapy with high doses of penicillin, tetracycline, erythromycin or clindamycin is necessary to prevent relapses.
Atypical mycobacterial lymphadenitis
Atypical mycobacteria typically present in the pediatric population as unilateral neck masses localized in the parotid or anterior neck triangle. There is induration, painful, red-brown skin. Diagnosis is made by culture and skin tests. The most common nontuberculous mycobacterium isolated from the neck in nontuberculous lymphadenitis is Mycobacterium avium complex. Tuberculin skin test (PPD) is often positive (10-15 mm. swelling), but a clearly positive test (>20 mm) is more valid for tuberculosis. Diagnostic criteria in a study are listed below; 1-positive PCR or culture, 2-positive skin test (PPD>6mm), 3-histopathological features consistent with mycobacterial infection and/or positive direct SMR for acid phase bacillus. Other criteria; chest X-ray normal, PPD<15mm, no contact with adult tuberculosis,
Complete surgical excision can be curative. Relapses usually occur after simple incision and drainage or incomplete excision. The greatest risk of surgery is marginal mandibular branch dysfunction of the facial nerve, a rate of 24.6% in a recent study. In treatment, drainage, curettage, excision and antibiotic therapy can be used in combination.
Tuberculous lymphadenitis (Scrofula)
It is the most common form of extrapulmonary tuberculosis. It is more common in adults than children. Existing lymphadenopathies are diffuse, bilateral compared to mycobacterial. The tuberculin skin test (PPD) is strongly positive (>20mm). The patient is often asymptomatic and does not show other signs of active tuberculosis. However, children and immunocompromised adults can suffer from co-occurring pulmonary diseases. Painful swellings, irregular ulcerated lesions, night sweats, and neck and mediastinal masses can be seen.
In the last 20-30 years, there has been a decrease in specific bacterial infections in Turkey. The most important of these is tuberculosis. Interestingly, pulmonary TB. decreased, there was an increase in extrapulmonary Tbc. The most common is Tbc.cervical lymphadenitis.
FNAB usually reveals granuloma and sometimes acid-alkali resistant bacilli. Specimen culture is important to distinguish TB lymphadenitis from forms caused by other mycobacteria and fungi. According to some clinicians, it is sufficient to see caseified necrosis in pathology for TB lymphadenitis. In bacteriological examinations such as SMR and culture, the result is negative in half of the cases due to the low number of bacteria. In countries where routine BCG vaccination is applied, such as Turkey, PPD positivity is neither latent nor active Tbc. does not mean infection
Tuberculous lymphadenitis treatment, known as scrofula, is an antituberculous medical treatment, although it depends on local sensitivity and culture results. Isoniazid and rifampin for 9 months, or isoniazid, rifampin and prazinamide for 6 months are sufficient.
Sarcoidosis
It is a multisystem disease that causes fatigue and weight loss, which is most common in the second decade of life. Most patients have pulmonary manifestations that regress spontaneously. Hilar adenopathy is seen on chest X-ray. Most of the clinical manifestations are related to the pulmonary system and nearby thoracic lymphatics. The clinical spectrum can concern any organ. Head and neck symptoms are detected in 10-15% of patients, the most common finding is cervical adenopathy.
Sarcoidosis is a chronic granulomatous disease, there are non-caseating granulomas for the involved organ. As physiopathology; Activation of cytokines and stimulation of T cells elicits macrophages with antigen as an immune response. Giant cell histiocytes are seen within sarcoid granulomas. There are CD4+ T cells in the middle of the granuloma and CD8+ cells in the epithelial margin.
In etiology; Although the exact cause of sarcoidosis is unknown, genetic factors, infectious agents and environmental factors may be effective.
At the initial diagnosis, one third of the patients are asymptomatic, while the other third have general symptoms such as fever, weight loss, and malaise. Clinical suspicion begins with a persistent dry cough, eye or skin manifestations.
Depending on the severity of the disease, corticosteroids can be used in the treatment.
Kimura's disease
Kimura's disease may also be called eosinophilic lymphogranuloma or eosinophilic hyperplastic lymphoganuloma. In 1948, Kimura and Ishikawa gave this name in Japan.
It is a chronic inflammatory disease of the head and neck, primarily in Asian men. Triple triad: 1- Painless unilateral cervical adenopathy, 2- Blood and tissue eosinophilia, 3- Obvious serum IgE elevation
It occurs as tumor-like subcutaneous nodules involving the major salivar glands and regional lymph nodes. Etiology is unknown, allergic and autoimmune theories have been suggested.
On USG, they are hypoechoic masses with hairy appearance created by hyperechoic bands.
Treatment: Conservative surgical excision at initial diagnosis, 25% recurrence. Observation if there are no symptoms or signs. Intralesional or oral steroids are used in non-cycles.
FUNGAL INFECTIONS
Fungal infections in the neck may develop in immunocompromised patients. The most common organisms are Candida, Histoplasm and Aspergillus. Serological and fungal cultures make the diagnosis. Aggressive, systemic antifungal therapy such as amphotericin-B is used.
NONE-INFECTIOUS INFLAMMATORY NECK MASSES
Rosai-Dofman disease (Sinus histiocytosis)
It was first described in 1965. Children have massive, non-tense cervical adenopathy, fever, and skin nodules. It is characterized by benign self-limiting lymphadenopathy. It is a rare disease and the cause is unknown, it has been stated that it may be due to idiopathic, herpes or viral infection such as Ebstein-Barr. There is extranodal involvement in 40% of the cases, mostly the skin, nasal cavity and paranasal sinuses are involved. biopsy; classically shows dilated sinuses, plasma cells, and histiocyte proliferation. Histiocyte cytoplasm contains intact lymphocytes. Limited local LAP is surgically removed. Corticosteroids are the first choice in multiple and systemic nodal disease. Other choices are immunomodulators or stotoxic chemotherapy.
Kawasaki disease
It is an acute multisystem vasculitis disease in children. Patients have several symptoms; acute, cervical lymphadenopathy, erythema, edema, exfoliation of the hands and feet, polymorphous exanthema, conjunctival infection, erythema of the lips and oral cavity. Diagnosis is made by clinical signs. Aspirin and immunoglobulins are used in treatment. It is a rare disease and cardiac complications may develop.
Castleman's disease
This disease is rare and is a potentially benign lymphoepithelial disease for the development of Kaposi's sarcoma and lymphoma. It peaks in the second and fourth decades. It is most common in the thoracic lymph nodes (70%), followed by the pelvis, abdomen, retroperitoneum, skeletal muscles, and head and neck (15%). Most neck lesions are unifocal. It has been reported very rarely extranodally in the parotid, submandibular gland, parapharyngeal area, floor of the mouth, and larynx. Its size is 5-10 cm in diameter, in the form of a solitary, ovoid neck mass. In contrast-enhanced CT, there is clearly homogeneous involvement in the middle, and a heterogeneous increase in the periphery is rarely seen.
Clinically, it is a unifocal asymptomatic mass. General symptoms in plasma cell type may include fever, diarrhea, weakness, weight loss, hepatosplenomegaly, and hematological findings.
FNAB is the best diagnostic method for the diagnosis of lymphadenopathy. In cytology; hyaline vascular type (90%) or plasma cell type (10%) are seen.
Treatment is surgical and full cure is provided. Radiotherapy and chemotherapy are considered as supportive in unresectable, incomplete resection, recurrence cases)