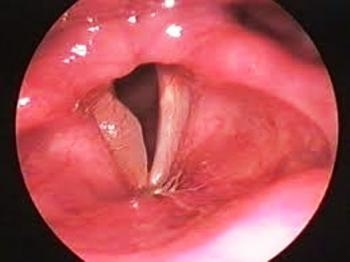
Vocal cord paralysis is a voice disorder that develops as a result of damage to the vocal cord nerve for various reasons or compression due to pressure and edema, poor functioning of the vocal cord or inability to work at all, and/or shortness of breath and breathing problems. Common causes of paralysis include goiter surgery, thoracic cage surgeries, lung, esophagus and thyroid gland cancers, and viral upper respiratory tract infections. In goiter surgery, the vocal cord nerve can be damaged unilaterally or bilaterally. The left vocal cord nerve may be damaged in surgeries in which the thoracic cage is opened. In cancers of the lung, esophagus, and thyroid gland, the tumor compresses or destroys the vocal cord nerve. In viral upper respiratory tract infections, the virus inflames the nucleus of the vocal cord nerve in the brainstem and prevents it from functioning; the cause of this type of vocal cord paralysis is unknown, only guessable; This type of paralysis usually heals spontaneously. Vocal cord paralysis can be unilateral or bilateral.
In the unilateral one, the vocal cords cannot come together during sound production and there is a gap between them; Because of this gap, there is a lot of air leakage while the patient is talking. The sound reproduction is demanding, the sound quality is rather distorted and breathy. Voice and cough are weak; the patient can speak for a very short time; He needs to breathe often. In bilateral vocal cord paralysis, shortness of breath with effort occurs because both vocal cords are close to the midline and cannot be opened to the sides. The patient becomes choked while carrying a light load or climbing stairs and has respiratory distress. His voice is monotonous; He cannot make his voice thinner or thicker.
However, the patient's main complaint is shortness of breath; They don't complain much about the sound problem. Sometimes swallowing difficulties may accompany it; The patient may have a coughing attack while drinking liquid, as the liquid escapes into his lungs.
Diagnosis is made by otolaryngological examination, fiberoptic endoscopy or stroboscopy. In stroboscopy, immobility of the vocal cord or cords is observed; a gap remains between the vocal cords, which are unilateral; In bilateral cases, it is found that the vocal cords remain immobile in the midline and the respiratory passage is considerably narrowed. 3-4 weeks after vocal cord paralysis, electromyography (EMG) is performed on the larynx muscles to obtain information about the cause of the paralysis, the location of the paralysis and its healing potential. A new EMG is performed 4 weeks after the first EMG, and signs of improvement or degeneration are investigated. EMGs performed 6 months after the onset of the paralysis are meaningless. Voice therapy can be very helpful for unilateral vocal cord paralysis. In voice therapy, the patient is given exercises to bring the vocal cords closer together. In this way,
However, the treatment of vocal cord paralysis is surgery. The patient is followed up for 6 months after the paralysis occurs; During this time, no permanent surgical intervention is performed. During this period, the stroke is expected to heal on its own. If there is no improvement, surgical interventions are considered.
In unilateral vocal cord paralysis, surgeries are performed that push the paralyzed vocal cord towards the midline, as the paralyzed vocal cord cannot reach the midline and stays on the side and cannot contact the other vocal cord.
Treatment methods:
1. Intrachordal injection (with fillers)
2. Medialization (Tyroplasty)
3. Neuromuscular surgery
4. Phoniatric therapy
In bilateral vocal cord paralysis, the aim is to widen the airway. Treatment methods:
1. Endoscopic arytenoidectomy (Thornel),
2. Transcervical arytenoidectomy (Woodman),
3. Posterior cordotomy,
4. Medial arytenoidectomy and thyroplasty type 2 (lateral) operations are performed.
In addition, definite voice rest is done; that is, communication should be made without speaking, only by writing, not even whispering. Drink plenty of water, moisten the larynx with cold steam, and abandon the throat clearing behavior. Mucolytic drugs can be used to soften saliva. Cortisone should never be given for early recovery of the voice.